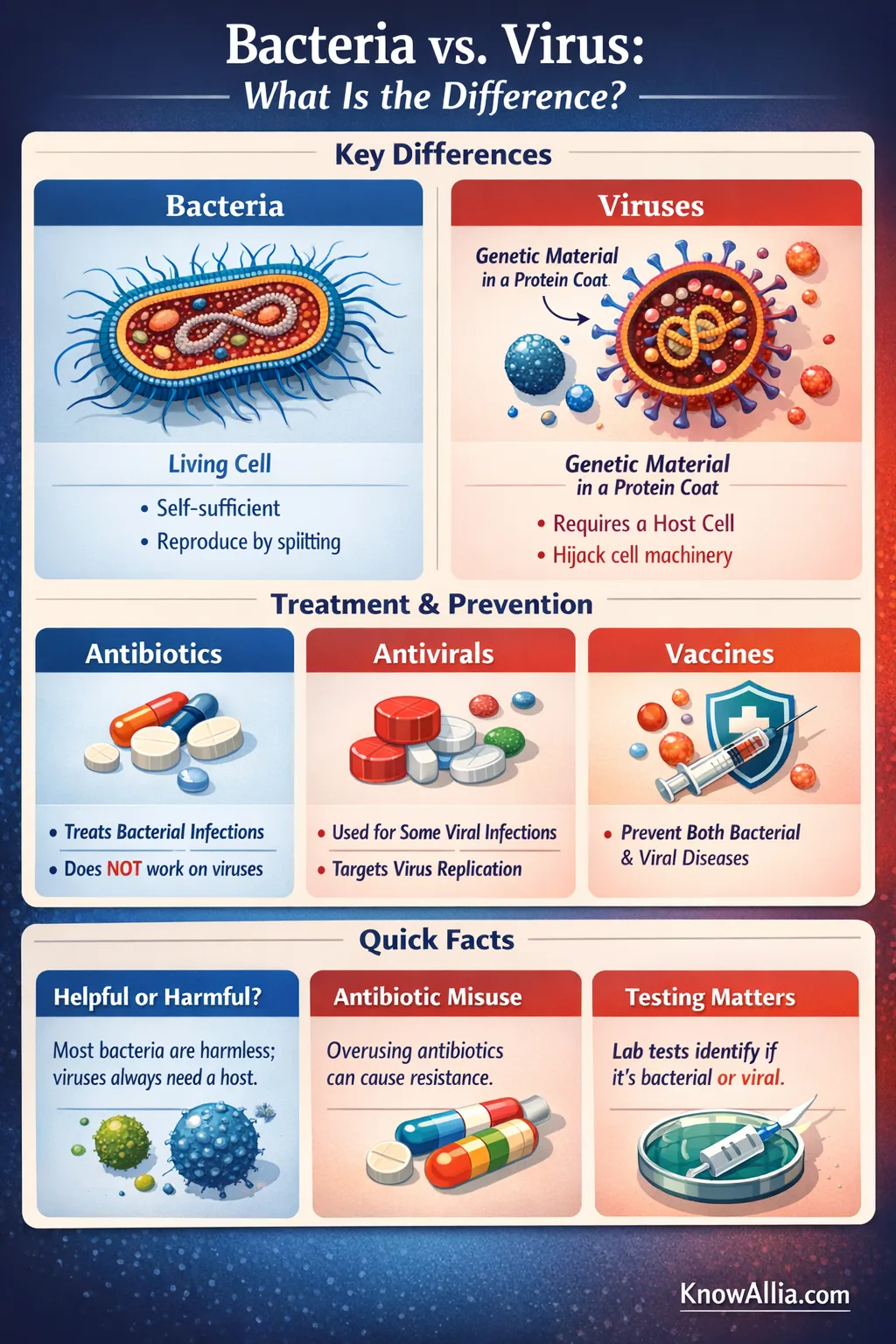
Bacteria are living, single-celled organisms, while viruses are infectious particles made of genetic material wrapped in a protein coat that must use a host cell to make copies of themselves.[a]🔗[b]🔗
A Clear Way to Think About It
Bacteria are complete cells with their own machinery. Viruses are genetic instructions in a protective shell. That single difference explains how they multiply, what medicines work, and why lab tests look for different clues.
You’ll learn what bacteria and viruses are made of, how each one works, what “bacterial vs viral” really means in real-world illness, how testing helps tell them apart, and where the line can get blurry.
This is general education, not a diagnosis. If symptoms are severe, unusual, or not improving, a licensed clinician can help decide what testing or treatment makes sense.
What Bacteria and Viruses Are
Bacteria
Bacteria are cells. They have a cell membrane and the internal tools needed to take in energy, build proteins, and reproduce.[a]🔗 Many are harmless, and plenty are genuinely helpful—especially in ecosystems and in the human body.[a]🔗
- Cell Living organism
- Self-sufficient Has its own machinery
- Reproduction Usually divides into two (binary fission)
Viruses
Viruses are not cells. A virus is a piece of genetic material (DNA or RNA) inside a protein coat, and sometimes an outer envelope. It cannot replicate alone; it must enter a living cell and use that cell’s components to make new viruses.[b]🔗
- Particle Not a cell
- Dependent Needs a host cell to copy itself
- Replication Uses the host’s machinery
Core Differences That Matter
If you remember one mental picture, make it this: bacteria are like a fully equipped workshop that can run on its own; a virus is more like a USB drive of instructions—useful only when it plugs into a computer that can execute the code. That’s why viral infections and bacterial infections respond to different tools in medicine, and why confusion around antibiotics is so common.[c]🔗
| Category | Bacteria | Viruses |
|---|---|---|
| Basic Nature | Living single-celled organisms[a]🔗 | Infectious particles that must use host cells to replicate[b]🔗 |
| How They Multiply | Often divide into two; growth happens within the bacterium itself | Enter a host cell, hijack processes, assemble new virus particles |
| What Medicines Target | Some infections respond to antibiotics[d]🔗 | Some infections respond to antivirals; antibiotics don’t treat viruses[c]🔗 |
| Common Lab Clues | Culture growth, microscopy, certain blood markers (depends on illness) | Genetic tests (like PCR), antigen tests, antibody patterns (depends on timing) |
| Prevention Options | Vaccines exist for some bacteria; hygiene and food safety matter | Vaccines exist for some viruses; hygiene and ventilation can matter too[g]🔗 |
Bacteria and Viruses, Side by Side
One is a self-running cell; the other is a set of instructions that needs a host. This snapshot shows what changes because of that.
How They’re Built
What Changes Because of This
Bacteria usually multiply by dividing. Viruses assemble new particles after using a host cell’s machinery.[b]🔗
Antibiotics are for certain bacterial infections. They don’t treat viruses, which is why “viral vs bacterial” matters for prescribing.[c]🔗
Vaccines work by training the immune system; which vaccines exist depends on the specific disease (some are bacterial, some viral).[g]🔗
Helpful vs Harmful
Most bacteria are harmless, and many support normal life processes. Viruses are best understood as agents of infection that need hosts to reproduce.[a]🔗[b]🔗
Why Misuse Matters
Using antibiotics when they aren’t needed can push bacteria toward resistance, which makes some infections harder to treat later.[f]🔗
Testing Closes the Gap
Symptoms can overlap. Clinicians often rely on context plus lab tests to choose the right approach.[e]🔗
How Bacteria Operate
Bacteria are producers. They can take in nutrients, make proteins, and maintain themselves as living cells. Many kinds live in and on the body as part of normal life, and most do not cause illness.[a]🔗 When certain bacteria do cause infections, the infection often comes from the bacterium growing and triggering inflammation, toxins, or tissue irritation—how that plays out depends on the specific bacterium and where it’s growing.
Common ways bacteria live and spread (high-level):
- Free-living in soil, water, or surfaces
- Community living in biofilms (groups sticking to a surface)
- Host-associated as part of a normal microbiome
How Viruses Operate
Viruses are dependent by design. They carry genetic instructions, but they don’t have the full set of tools needed to build proteins or copy their genome on their own. To make more viruses, a virus must enter a living cell and use that cell’s components for replication and assembly.[b]🔗 That’s why viruses are often described as host-driven: the host cell is doing much of the work, just under new instructions.
A Simple Virus Life Cycle (Conceptually)
- Attachment: the virus binds to a specific type of cell.
- Entry: it gets inside (or injects genetic material).
- Copying: the cell’s machinery helps make viral components.
- Assembly: new virus particles are built from those components.
- Exit: new viruses leave to infect other cells.
Illness and Treatment: Why the Difference Matters
Many symptoms—fever, fatigue, sore throat, cough, stomach upset—can show up in both bacterial and viral illnesses. That overlap is the reason testing and clinical context matter. A careful review of symptoms plus lab tests can help guide treatment choices.[e]🔗
Antibiotics
Antibiotics are designed to target bacterial features (like how bacteria build cell walls or make proteins). They do not work on viruses.[c]🔗 Even among bacterial infections, antibiotics aren’t always needed for every situation, and the best choice depends on the illness and the person.[d]🔗
Antivirals and Supportive Care
Some viral infections have antiviral medicines that can slow replication or reduce severity when used appropriately, while many viral illnesses are managed with symptom relief and time. Clinicians may combine this with prevention strategies like vaccination, when available.[e]🔗[g]🔗
There’s another reason the distinction matters: using antimicrobial medicines when they aren’t needed can encourage resistance over time, making some infections harder to treat later. This is a global issue, and it’s one reason clinicians try to match the right medicine to the right cause.[f]🔗
How Tests Help Tell Bacteria and Viruses Apart
“Bacterial” and “viral” are categories, but real-life diagnosis is usually more specific: which organism, in which location, at what stage of illness. Because symptoms can overlap, lab tests are often used to narrow things down.[e]🔗
Common Test Approaches (Broadly)
- Culture: some bacteria can be grown in a lab from a sample, which helps identify them and guide treatment.
- Rapid antigen tests: look for pieces of an organism (often used for some viruses, and sometimes bacteria depending on the test).
- Genetic tests (like PCR): detect genetic material from a virus or bacterium, often with high sensitivity (timing matters).
- Antibody tests: show how the immune system responded; these can be more useful for certain questions after an infection has progressed.
In practice, clinicians often combine pattern recognition (symptoms, exposure context, how quickly things started) with testing. When it’s hard to separate bacterial from viral based on symptoms alone, lab work helps reduce guesswork.[e]🔗
Prevention and Protection
Prevention is less about “bacteria vs virus” and more about breaking transmission chains. Some tools work broadly (like hygiene), while others are specific (like vaccines for particular diseases).[g]🔗
Vaccination
Vaccines help the immune system learn what to recognize, so it can respond faster later. Which vaccines exist depends on the disease; some prevent bacterial diseases, some prevent viral diseases, and some communities use schedules to keep protection up to date.[g]🔗
Everyday Barriers
Basic measures—like good hand hygiene and avoiding close contact when sick—can reduce spread for many infections. Clinical guidance often emphasizes these behaviors because they help across a wide range of causes.[e]🔗
Common Misconceptions and Mix-Ups
Common Mix-Up
“Antibiotics help with colds if the mucus is thick or colored.”
What’s True
Antibiotics don’t treat viruses, even if mucus changes color. Treatment depends on the cause and the clinical picture.[c]🔗
Common Mix-Up
“Bacteria are always ‘bad’ and viruses are the only germs that matter.”
What’s True
Most bacteria are harmless, and many are helpful in ecosystems and in the body. A smaller number cause disease.[a]🔗
Common Mix-Up
“If it’s viral, there’s nothing medicine can do.”
Key Terms
- Pathogen
- An organism or infectious agent that can cause disease.
- Host Cell
- A living cell a virus uses to make copies of itself.[b]🔗
- Antibiotic
- A medicine used to treat or prevent certain bacterial infections; it does not treat viral infections.[d]🔗
- Antimicrobial Resistance
- When microbes change over time and medicines become less effective; it can involve different types of microbes and treatments, including antibiotics and antivirals.[f]🔗
- Vaccine
- A product that trains the immune system by imitating infection in a controlled way, helping protect against certain diseases.[g]🔗
- Microbiome
- The community of microbes that live in and on the body; many bacteria are normal and helpful parts of it.[a]🔗
Where the Edges Get Fuzzy
The bacteria-versus-virus distinction is solid, but real life adds nuance. Symptoms can overlap, some illnesses can be caused by either category, and timing can change what a test detects.[e]🔗 It’s also possible to have more than one infection at once, which can complicate the picture.
Science also keeps learning new details about how microbes interact with the body. For example, researchers continue to refine how the microbiome influences immunity and inflammation, and how resistant strains emerge and spread over time.[f]🔗 When evidence is still evolving, good clinicians and good public-health guidance usually lean on what is most reliable: clear diagnosis, appropriate treatment, and prevention.
FAQ
Questions People Often Ask
Are viruses “alive”?
Viruses are not cells and can’t replicate on their own. They must infect a host cell and use that cell’s components to make new viruses.[b]🔗
Why don’t antibiotics work for viral infections?
Antibiotics target bacterial structures and processes. Viruses don’t have those same targets, so antibiotics don’t treat viral infections.[c]🔗
Can vaccines prevent both bacterial and viral diseases?
Yes. Vaccines exist for some diseases caused by bacteria and for some caused by viruses. Availability depends on the specific disease and vaccine development.[g]🔗
How do clinicians decide if an illness is bacterial or viral?
They often combine symptoms, timing, exposure context, and laboratory tests to guide treatment. Some conditions can be caused by either type, so testing helps reduce uncertainty.[e]🔗
What is antimicrobial resistance in simple terms?
It’s when microbes change over time and medicines become less effective, which can make infections harder to treat. Using antimicrobials appropriately helps slow this trend.[f]🔗
Are most bacteria harmful?
No. Many bacteria are harmless, and some are helpful. A smaller number of bacterial species cause disease.[a]🔗
Sources
- [a] National Human Genome Research Institute (NIH) – Genetics Glossary: Bacteria (Definitions and background on what bacteria are.)
- [b] National Human Genome Research Institute (NIH) – Genetics Glossary: Virus (Definition and the idea that viruses must use host cells to replicate.)
- [c] Centers for Disease Control and Prevention (CDC) – “Antibiotics Aren’t Always the Answer” (PDF) (Why antibiotics don’t work on viruses; antibiotic-use basics.)
- [d] NHS – Antibiotics (What antibiotics do, what they don’t do, and why appropriate use matters.)
- [e] Mayo Clinic – Bacterial vs. Viral Infections: How Do They Differ? (Clinical perspective: overlapping symptoms, role of lab tests, prevention ideas.)
- [f] World Health Organization (WHO) – Antimicrobial Resistance (Fact Sheet) (What resistance is and why appropriate antimicrobial use matters.)
- [g] CDC – Vaccine Basics (How vaccines build immunity; general vaccination context.)